Compare providers
Download our outplacement comparison sheet
Request pricing
Compare our rates to other providers
Here’s a cold, hard fact: Americans are more likely to die of an opioid overdose than a car crash. Every day, an estimated 130 people die because of these overdoses across the country.
It’s safe to say that the opioid epidemic is still in full swing with no end in sight. Not only does the public health crisis threaten lives, families, and the economy, it’s also plaguing HR departments who see the problem but can often times feel powerless to help.
But what can HR do during these trying times? After all, given the figures and anecdotal experiences, we all probably know someone who has battled with opioids or has even died because of them. This means that most, if not all, of our employees have similar stories. So how can we help?
This question is complex to say the least. To help HR navigate this, we’ve decided to do a deep dive into the opioid crisis to examine what top thought leaders are suggesting and what things HR can – and cannot – do to help their staff members.
Let’s get started with some history about the problem itself.
The Opioid Crisis: A Brief History
Even though HR leaders don’t have to be an expert on the opioid crisis, it helps to understand where the problem started because, later on in this article, it’ll be important.
The opioid crisis is believed to have stemmed from the over prescription of pharmaceutical pain killers, such as Vicodin and others. Typically, a person is prescribed a large amount of pain killers to help with issues such as back pain, a tooth ache, or really anything that hurts.
The person starts using these drugs to keep performing their daily functions without the constant pain. However, because they have so many pills and because they are so addictive, they quickly get hooked on them. This creates a vicious cycle that can eventually lead to people overdosing on prescription drugs, turning to heroin, and other things – none of which are any good.
This problem was mainly caused by the fact that drug companies promised doctors and patients that opioids were not addictive.
“In the late 1990s, pharmaceutical companies reassured the medical community that patients would not become addicted to prescription opioid pain relievers, and healthcare providers began to prescribe them at greater rates,” reports the National Institute on Drug Abuse (NIDA).
“This subsequently led to widespread diversion and misuse of these medications before it became clear that these medications could indeed be highly addictive. Opioid overdose rates began to increase.”
With drug companies lying to the public, the opioid crisis exploded, impacting just about every community in America. NIDA reports that in 2017, 47,000 people died as a result of opioid overdose. Also in that year, a whopping 1.7 million people suffered from opioid substance abuse.
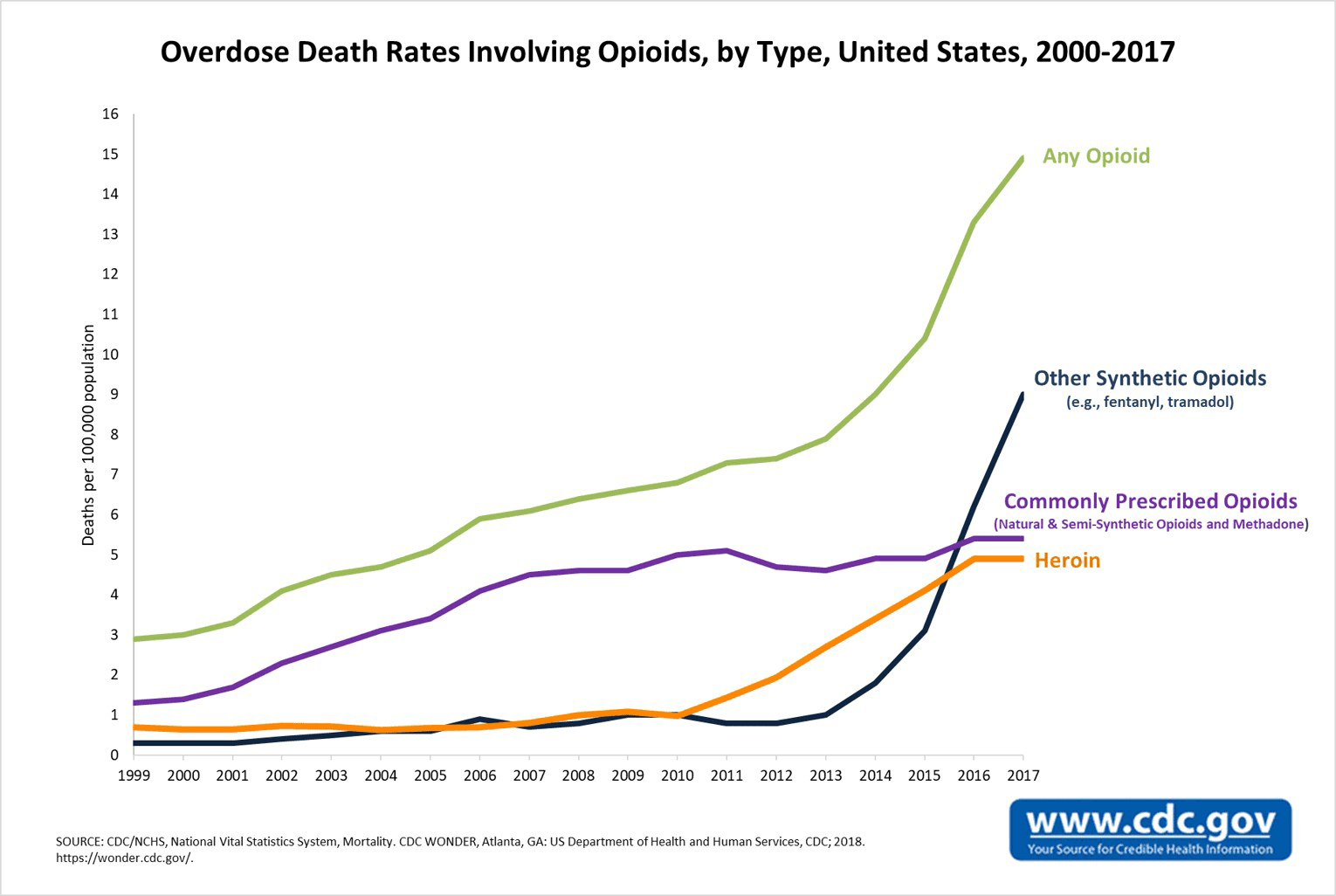
They do not report on 2018 or 2019, though it seems safe to assume that the problem continued to rise. Here’s a chart that shows the increase of overdoses from the 1990s to 2017:
To help explain this further, here are some quick stats that help paint a picture of how wide-spread the problem is (all figures come from NIDA):
- 21 to 29 percent of people prescribed opioids for pain misuse them
- Eight to 12 percent of people prescribed opioids develop a use disorder
- Four to six percent of these people eventually transition to heroin
- 80 percent of heroin users first misused opioids
- From July 2016 to September 2017, overdoses spiked by 30 percent
- In that same time, the Midwest region saw a 70 percent spike in overdoses. In large cities in 16 states, a spike of 54 percent occurred.
As you can clearly see, most – if not all of America – has been touched by this problem. If not us personally, we all most likely know someone who has struggled or even passed away because of this crisis.
Now that all of the facts and history is out of the way, what can HR do in the face of the problem? Is there anything actually beneficial for HR departments to do, or is the problem too vast?
Let’s dig in.
Most HR Departments Know There’s a Problem and Feel Unprepared to Help
Though we just explained the opioid problem in detail, we probably didn’t have to, according to a 2018 survey by The Hartford. They report that 67 percent of HR leaders reported knowing that there was an opioid problem in their workplace. However, they also found that 76 percent of employees and 64 percent of HR leaders don’t feel that they are well-trained enough to help their coworkers.
“Just 24 percent of HR professionals and 18 percent of employees in the survey felt ‘very’ or ‘extremely’ confident that they could recognize the signs of opioid addiction, and only 19 percent of HR professionals and employees felt ‘very’ or ‘extremely’ aware of how to minimize the risk of addiction,” reports HR Drive.
That’s a startlingly high percentage. Basically, the company, the employees, and HR all know that some workers may be struggling with opioids, but the large majority of them feel powerless.
So, why does HR feel so helpless? There aren’t too many in-depth studies looking into this, but it’s most likely because the problem is extremely personal and also just plain hard to talk about. It can be hard to even bring these problems up to a loved one let alone an employee who you may not be all that close with.
Despite this challenge, there are some things HR can, and should, consider doing, such as:
Examine Poor Health Plans
One of the most important things is looking into the company’s benefits packages. Remember that much of this crisis started with a visit to the doctor – typically for some sort of chronic pain, such as a sore back.
“One hundred fifty-five million Americans have employer-provided health insurance and because of this, employers are unwitting enablers for the sad state our healthcare system is in today, opioid crisis included,” writes Dave Chase, co-founder of Health Rosetta, in an article for HR Drive.
“Employers have been maintaining the status quo, providing poor healthcare coverage (that is often quite expensive) and failing to realize that doing so could have a profoundly negative impact. For example, employees continue to receive opioid prescriptions for lower back pain despite there being no evidence of their effectiveness (other than temporarily masking pain).”
Chase argues that many of these doctors who are part of lower tier health plans simply ignore the root cause of pain and instead slap a prescription down as a viable means of solving it. In other words, sure, a painkiller will likely help your tooth ache feel a lot better, but – at the end of the day – you still need to fix the tooth. The pain is just a signal telling your body that something is wrong.
“The silver lining, however, is that employer-provided health insurance — which has historically been part of the problem — can also be a salvation,” Chase continues.
“By offering employees access to value-based care models like direct primary care, employers can save money and stop addiction before it starts, minimizing the opioid crisis’ impact on their workplaces.”
In short, a big step in the right direction for HR departments is to find health plans that are actually value-based. Most of the time, given our current system, if you have a back problem and want to seek medical attention, you will either have to go to the ER, which can be costly even with a healthcare plan, or make an appointment with a doctor.
If you go the latter route, you may have to wait a little bit to be seen. Once in there, some doctors will want to turn you around as fast as possible to get you back to work. This is where the opioids come into play.
Not only does this introduce drugs into the equation, it doesn’t fix the underlying problem, which can then cause more drug use and the actual injury to worse. Over time, you can see how this becomes a vicious cycle that, for some, can lead to overdoses and heroin use.
Those are big stakes. And they all come down to choosing a healthcare plan for workers. Now, it can be quite challenging for HR and companies in general to fully vet every doctor inside a healthcare plan.
Without getting way into the weeds about various healthcare models, Chase suggests that employers should simply look into ‘value-based’ models.
“To give employees this kind of high-quality care, employers should first find out if their benefits brokers have experience working with value-based primary care practices (the good ones do) and if they do not, encourage them to research which primary care organizations would be able to provide such services,” he writes.
To learn more about these programs, we highly suggest that you read his full report.
Teaching Employees to Spot the Signs of Addiction
While paying closer attention to healthcare plans will do wonders, HR should also train staff members (and themselves) how to recognize the signs of opioid addiction, too.
At the annual SHRM conference back in 2018, Norbert Alicea and Raffi Terzian shared with attendees a presentation called Addressing Prescription Overuse in the Workplace.
Their talk centered on quite a few things that HR should pay attention to when it comes to opioids. One of which was how important it is for employers and employees to notice the signs.
“Alicea addressed the necessity for more thorough training so managers and supervisors are better equipped to recognize the red flags,” reports David Shadovitz for Human Resource Executive.
“They need to be able to identify the early warning signs, such as absenteeism on Mondays and Fridays (or the day after a payday), lateness, poor quality of work, theft, and morale.”
He goes on to say that workers, on the staff level, always know these things far earlier than upper management, which makes sense because these workers are more intimately connected with their peers.
“I can’t even tell you how many times an HR person has called me about a problem employee who has tested positive, even though it has been going on for five years,” said Alicea, according to Shadovitz.
“HR needs to help the managers and supervisors understand that this is a real issue and teach them how to supportively confront employees, including what to say and what not to say. That’s where HR can come in as a partner, helping them focus on identifying the early warning signals and helping them remain objective.”
Even though identifying individuals who may be suffering from opioid addiction is a good first step, it can be challenging both personally and legally to get too involved.
For one thing, confronting someone about an addiction of any kind will likely not be met with excitement from the individual. Alicea says that the key here is to use ‘I messages’ that do not directly confront the person.
For example, someone could say, “I am concerned about your work performance” or something along those lines. On the other hand, you shouldn’t come at the perqson with, “You’re an addict. You have a substance abuse problem.” That’s just going to start a confrontation.
He also says that after these statements it’s okay to send the staff member for a ‘medical evaluation’ (read: drug test) to see what’s going on.
Another important takeaway from the talk was the fact that threatening someone’s job over opioids is likely the wrong move. After all, when you threaten someone’s job or straight up fire someone because of their addiction, you may (will) stress them out even more, which can lead to a whole bunch of things – none of which are good outcomes.
This is where a ‘last-chance agreement’ can come into play. By allowing your employee to get help and beat their addiction, providing them a support system in the process, you can retain them and literally help them get through this situation.
There’s obviously a business case for this, too, which rings inhuman, but would be nonsensical to not notice. Firing people, searching for talent, onboarding, training, and eventually fully replacing workers is never a cost-effective move. Why not retain the employee and provide assistance at the same time? Create a win-win.
And, we just have to say it, you should want your staff members to beat their addiction not only because of their work but because they are a person in need of support (you know this, but we have to reiterate).
With all of that said, like we mentioned above, it can still be very tricky to approach someone who you think may be struggling with addiction. Not only on a personal level but a legal level, too.
Confronting Staff Members: What You Need to Know
Confronting a staff member about drug use is never easy, but HR and management do have systems in place to do so.
This is all really tied up to how your company’s policies are written. For example, you may have a policy that allows for random drug testing and things like that. The most common way drug tests are administered is performance-based.
In this situation, let’s say that someone came to HR and reported an employee who seems to be under the influence of a drug or alcohol. HR can call that employee in and if they notice anything suspicious they can administer a drug test.
Sometimes, if the employee does have an addiction, they may come out and say it before the drug test is performed. On the other hand, some will try to pass anyway.
There are some things that must be said here, though, before we get into the recovery stage. The Equal Employment Opportunity Commission (EEOC) makes it clear that employers should only be allowed to drug test individuals when there is probable cause that the use will impact job performance and/or safety.
This means that you shouldn’t drug test on rumor alone because it can land you and the company in hot water.
Kathryn Russo, an attorney with Jackson Lewis in New York, talked to SHRM about this issue last year.
“Many employers are expanding their drug-testing panels to include semisynthetic opioids such as hydrocodone, hydromorphone, oxycodone and oxymorphone, in addition to traditional opioids such as heroin, codeine and morphine,” she said, according to SHRM.
“This is lawful in most states as long as the employer does not take adverse employment actions when drugs are used legally, she noted, which is why an employer should use a medical review officer in the drug-testing process. If the medical review officer concludes that the positive test result is the result of lawful drug use, the result is reported to the employer as negative.”
Now, if a drug test is done correctly like Russo explains above and comes back positive or a person admits to having an addiction before the test, there are a few options now on the table.
The first option is to forgo disciplinary action and instead have the employee go through impatient treatment for their addiction. According to experts, this is the wrong way to go because ‘employers are not doctors.‘ This makes a lot of sense. Employers may be alerted of the issue but they cannot accurately assess the person’s state. That should be left to professionals who can help employees through these trying times.
This is where employee assistance programs can come in very handy. You can learn all about those here.
So far, we’ve covered what can happen if an employer drug tests an employee, but you should also be careful when in these situations because employees may have voluntarily sought out help. Some states, such as California, require employers (usually of a certain employee size) to accommodate drug and alcohol recovery programs, SHRM reports.
Still, even if a drug test was used, employers are capable of making agreements with the employee that they can keep their job and receive no disciplinary action as long as they receive treatment. It’s important, though, that employers allow professionals to work with the employee and have a barrier between them.
“The employer may choose to forgo disciplinary action if an employee agrees to these terms and signs an agreement to this effect. The employer then would not have to be informed about the person’s decided course of treatment, whether inpatient, outpatient or no treatment at all,” said Nancy Delogu, an attorney from Littler in D.C., according to SHRM.
“The employee typically will be subjected to follow-up drug testing to make sure he or she hasn’t resumed the use of illegal drugs.”
SHRM also says that employers should never outright accuse someone of having an addiction. We mentioned this above, but there are legal issues that forbid this as well. For example, if the person is already seeking treatment, you may be violating the Americans With Disabilities Act.
For example, an employee with a health condition may take prescription drugs for that issue. Or, they could have a history of drug and alcohol abuse. Either way, the solution here is to simply never outright accuse someone because it can lead to ADA claims and – like we said before – really gets the whole conversation started on the wrong foot even if there is no ADA violation.
The Opioid Crisis and HR: The Takeaways
As you probably know, the opioid crisis is complex and can be quite confusing for HR leaders to deal with. Given the complexity, it’s no surprise that many HR leaders and managers feel unprepared even though they know that their workforce is likely suffering from the crisis.
There are some good steps that HR leaders can take, though. One of the biggest is looking at healthcare programs to see if doctors are over prescribing pain killers for ailments. This is where the crisis is believed to have started. So, by stopping it before it starts, HR and management can be at the cutting edge of the issue.
If an employee is struggling with opioids, make sure you follow the best practices when confronting them and getting them the help they need and deserve. Sensitivity is the name of the game here. You need to be on your employee’s side through this but also allow professionals to provide support and come up with treatment plans.
Like anything this complicated, we suggest that you come up with a policy for your workplace that works for you. Work closely with your legal counsel to ensure that you are complying with all regulations and local, state, and federal laws.
Insights and research
bring the CHALLENGE.
wE have the SOLUTION.
Protect your brand and support your people through change. From career transition to leadership development, we bring clarity and care to the moments that matter most.